Introducing ... Greenway Secure Cloud
Experience peace of mind, greater security, and all-inclusive pricing with Greenway Secure Cloud*.
Request Bundled Pricing

The Academy: You’ve been accepted!
With Cures Act requirements on the horizon, the
21st Century Cures Academy is your go-to destination for education and resources. EXPLORE THE ACADEMY
of Medicare beneficiaries have two or more chronic conditions.
of healthcare spending is attributed to patients with chronic conditions.
“You really have to know your practice and know your patient population. You also have to know which of the diagnoses included in the care plan would be most compelling for your patient population to participate in CCM.”

GRS Select™ — available now!
With our new, customizable revenue cycle offering, you can choose the services your practice needs the most. Customize your plan
"I know how hard it is to get everything in your 15 to 30 minute visit ... CCM was a new opportunity to connect with patients outside of the office visit.”

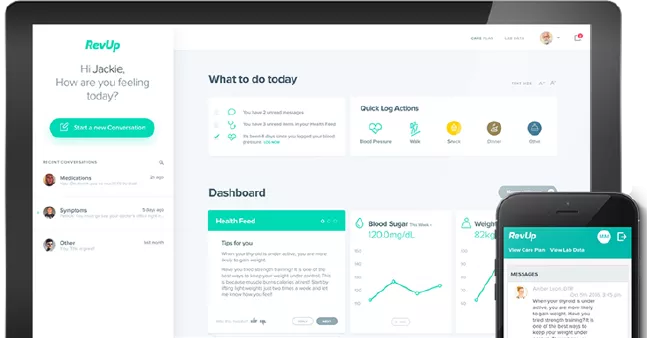
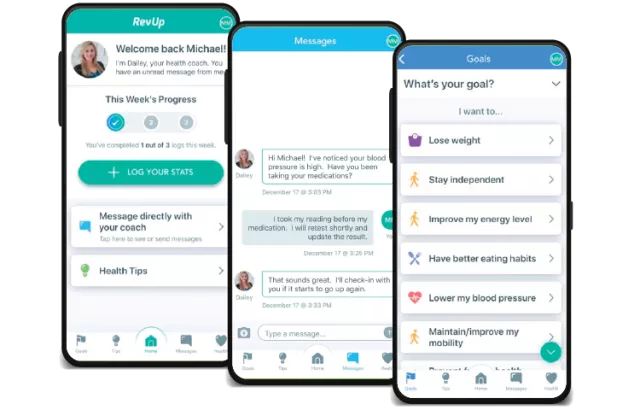
A complete suite of solutions to promote healthy outcomes
See how Greenway's integrated solutions keep your practice connected to patients in and out of the office.

Get additional care management tips in our Knowledge Center


How Greenway Health Stacks Up: A Competitive Analysis of Healthcare Technology Solutions


Solving Chronic Disease Management Problems With Telehealth


How Greenway Health Advances Equity in Tribal and Urban Indian Healthcare